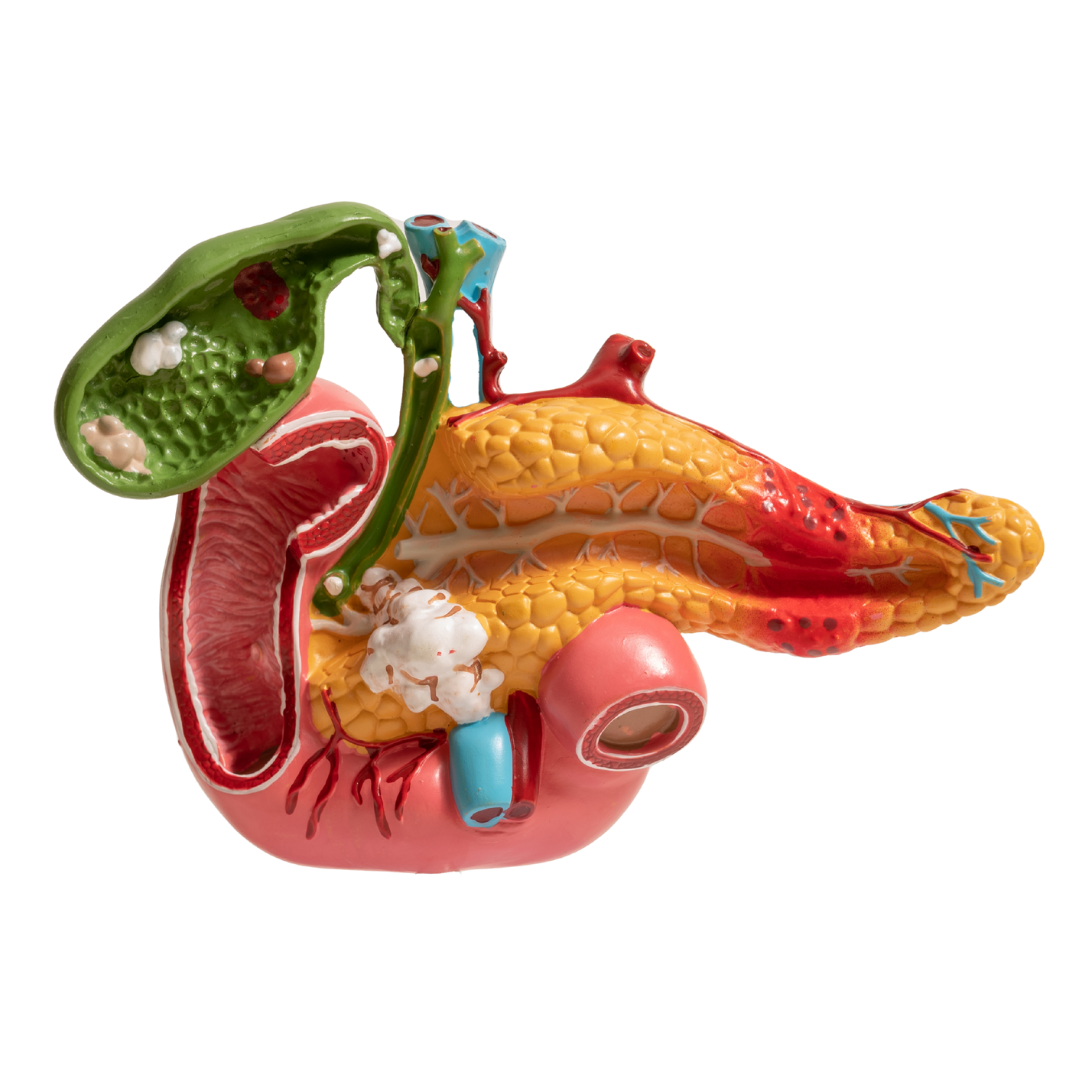
From steroid use to emerging therapies, understand your treatment options and relapse prevention.
Autoimmune pancreatitis (AIP) is a rare form of chronic pancreatitis driven by an abnormal immune response where the body’s own immune system mistakenly targets the pancreas, causing inflammation, swelling, and potential scarring of pancreatic tissue. This condition differs from typical pancreatitis caused by gallstones or alcohol, as it stems from immune-mediated mechanisms, including lymphocytic infiltration and elevated immunoglobulin G4 (IgG4) levels in its most common subtype. Histologically, it features dense lymphoplasmacytic infiltrates, storiform fibrosis, and obliterative phlebitis, hallmarks that distinguish it from other pancreatic disorders.
Common in men over 60, linked to IgG4-related systemic disease affecting multiple organs, presents with painless jaundice, elevated serum IgG4, and characteristic pancreatic inflammation high relapse after steroids.
Occurs around age 40, affects pancreas only, equally in men and women associated with inflammatory bowel disease normal IgG4 levels, granulocytic epithelial lesions on histology, lower relapse rate with steroids.
Caused by immune checkpoint inhibitor drugs in cancer therapy, often asymptomatic, CD8+ T-cell driven injury, poor steroid response, management balances therapy continuation and pancreatic inflammation.

Yellowing of skin and eyes, dark urine, pale or floating stools from blocked bile ducts.
Mild upper belly discomfort or pain radiating to the back, less severe than in typical pancreatitis, more common in Type 2 AIP.

Unexplained loss due to poor appetite, nausea, vomiting, or malabsorption, extreme tiredness is frequent.
Nausea, vomiting, feelings of fullness, or recurrent acute pancreatitis episodes in Type 2.
Dr. Vikas Singla brings over 20+ years of specialized experience Autoimmune pancreatitis disease treatment and Autoimmune pancreatitis disease diagnosis. Trained at AIIMS under renowned gastroenterologists and with international training from National Cancer Centre, Tokyo, he’s helped thousands of patients to recover in acute pancreatitis and reclaim their health.
Dr. Singla is an alumnus of AIIMS, New Delhi, and has helped thousands of patients overcome complex esophageal disorders.


The gastroenterologist reviews your medical history, symptoms, and performs a physical exam to assess your condition.

They order lab tests, imaging (CT, ultrasound, MRI), and may perform endoscopic procedures to diagnose and visualize abnormalities.

Based on results, a tailored plan is created including diet changes, medications, lifestyle adjustments, or surgery/endoscopic treatments if needed.

Regular appointments track treatment response, adjust care, and manage long-term conditions to prevent complications.
Oral corticosteroids are the primary treatment for AIP, starting at 0.6-1 mg for 2-4 weeks to induce remission, followed by gradual tapering based on symptoms and imaging response.
Long-term low-dose steroids reduce relapse risk, especially in Type 1 AIP, but may cause side effects like osteoporosis, infections, or steroid dependence.
Anti-TNF drugs and Janus kinase inhibitors show promise for steroid-resistant or relapsing cases, with biliary stenting used temporarily to relieve obstruction.
For steroid intolerance or relapse, immunosuppressants (azathioprine, mycophenolate, mercaptopurine) or biologics like rituximab are used to maintain remission effectively.
Therapy is individualized considering age, comorbidities, and disease severity. Early treatment reduces pancreatic damage and complications. Regular follow-up is needed to monitor relapse and adjust therapy.
Contact Dr. Vikas Singla to clear all your doubts related to Autoimmune pancreatitis. Whether you have questions about symptoms, treatment options, or recovery, we are here to guide you with accurate information and support.
The primary treatment is oral corticosteroids, like prednisone, which reduce inflammation and induce remission.
Yes, especially Type 1 AIP commonly relapses after stopping steroids, so maintenance therapy may be needed.
Side effects include osteoporosis, increased risk of infections, and potential dependence on steroids.
Yes, immunosuppressants and biologics such as rituximab may be used to maintain remission in steroid-intolerant or relapsing patients.
Mortality from AIP is rare, but risks increase with older age and other health conditions, mainly due to complications, not the disease itself.
Relapse is monitored through symptoms and imaging; treatment may include restarting steroids or other immune therapies.
Fields with * are required
